Clearing's Chronic Pain Blog
Pinched Nerve: The Different Types and How to Treat It
Jump To Section
You may know the feeling: it’s not throbbing, it’s not debilitating, but, well, it hurts. It may be in your back or neck and radiating to your arms or legs; it may have started following an intense workout or after a night of tossing and turning in bed. What is this feeling, exactly? Well, what you could be experiencing is a fairly common condition called a “pinched nerve.” And, although the pain sometimes goes away on its own (more on that later), it is essential to understand what you’re feeling, recognize your symptoms and pinpoint the cause of the pain. Remember, caring for yourself is priority number one. To do that, you need to be educated about your body.
For some context, our nerves can be thought of as nature’s version of fiber optic technology. The intricate system creates the vital connection between body and brain. This rapid-fire communication helps us to navigate, interpret and learn from every sensation and experience. Arranged in bundles of fibers, nerves conduct impulses of sensation to the brain and spinal cord while regulating and interpreting sensation for our muscles and organs.
Because they are so crucial to our survival, nerves are surrounded and protected by tissue such as bones, cartilage, muscles, tendons and the discs that cushion our backbone. But when this scaffolding buckles or weakens enough to apply excessive pressure, the nerve signals can become scrambled.
And this isn’t fun for anyone, since it can cause damage or inflammation that translates to strange tingling, intense stabbing pain, throbbing heat and sometimes, the worst: no feeling at all. This is known as a pinched nerve. In a nutshell, restoring function to a pinched nerve can involve building strength and flexibility, incorporating movement, getting rest and seeking medical attention.
What is a pinched nerve?
You’ve probably heard the term “pinched nerve” before, and that’s because it’s a blanket way of describing various conditions. To simplify the definition, a pinched nerve describes damage or injury to a nerve, or set of nerves, due to compression (tightening), constriction (narrowing), or overuse from the surrounding muscles.
A pinched nerve can feel like shooting pain, tingling, numbness and can sometimes be associated with weakness. Most commonly, pinched nerves occur in the neck or lower back. However, they can also take place in our wrists (just think of all that keyboard dancing you do!). There are many types of pinched nerves with unique names, including carpal tunnel and ulnar neuropathy. Here, we’ll focus on pinched nerves in the spine.
What does a pinched nerve feel like?
Sometimes, you’re simply sore from physical activity. Other times, you may have pulled a muscle. However, you’ll likely be able to detect a pinched nerve since it feels slightly different. One way to think about it is the sensation of your hand or foot falling asleep. It almost feels as if you’re walking on pins and needles, right? That feeling is the result of a mildly compressed nerve.
On the more extreme end, symptoms of a pinched nerve in your neck or back could feel like a similar tingling or any number of uncomfortable sensations. You may feel a sharp stabbing pain or burning sensation that shoots down your arm, back, or leg. You could also have muscle spasms or feel overly weak. Sometimes, you may feel like you’re numb, with little to no feeling at all.
How long does a pinched nerve last?
In most cases, with rest and proper stretching, you can usually get rid of a pinched nerve within a few days. However, a pinched nerve's symptoms can also last for a few weeks or months — or even longer. No matter the duration, it’s likely painful enough to sideline you from your activities.
Because of a pinched nerve's electrical sensation, it may cause you to worry it’s something more severe or potentially debilitating. Try your best to fight anxious thoughts since pinched nerves are not necessarily dangerous if they only last a few days. Rest and pain control with anti-inflammatory medications is often all that is needed while your body heals. However, if even after a few weeks the pain continues, your risk of chronic pain, limited mobility and nerve damage run higher and you should always consider talking to your doctor.
What are the different types of pinched nerves?
As we mentioned before, “pinched nerve” is a general term describing several health conditions. There are various “pinched nerve” diagnoses, including pinched nerves in the spine and in the periphery or outside of the spine. These all have different symptoms and require various levels of treatment.
Sign up for our newsletter
Learn more about our approach to whole-body pain relief.
We are covering the most common types of pinched nerve conditions, including:
- Radiculopathy
- Herniated disc
- Sciatica
- Pinched nerve in the neck
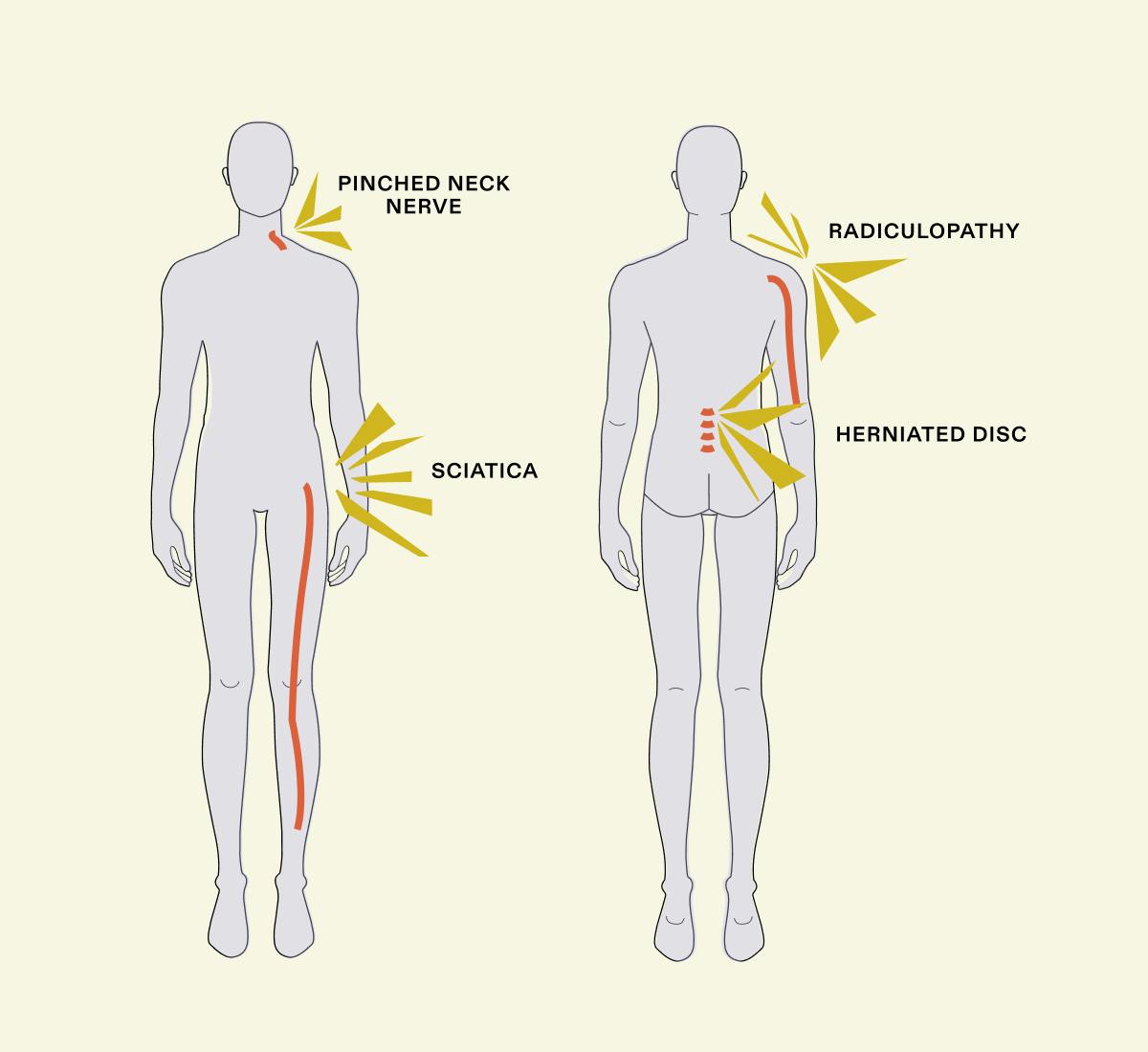
Radiculopathy
Our spines have to be both strong when we’re standing straight and flexible when we bend. Believe it or not, there are a whopping thirty-one pairs of nerves rooted in the spinal cord. They work together to control body movements and carry signals from the backbone to the brain. These nerve roots branch out from the spinal cord through tiny openings in the vertebrae.
Radiculopathy is an umbrella term that describes many symptoms that arise as the result of compression, constriction or irritation of nerve roots in the spine. The term itself comes from “radicular nerve,” which is another name for the lower back's nerve root. But what does the condition feel like? The answer could be a variety of sensations, including pain in the hip, shooting pain in the legs, intensified weakness, numbness and tingling. In terms of causes of radiculopathy, the most common is a herniated disc in the spine. Other causes include degenerative arthritis in the lower part of the spine, which narrows the spinal canal at the nerve exit.
Herniated disc
When you have a backbone, it means you have courage, grit and confidence. Or in other words, without one, we’d constantly be caving in instead of standing tall and strong. The same concept applies to anatomy. The vertebrae in our spine are sandwiched by discs that serve as cushions and shock absorbers, with a hard outer layer surrounding the center.
In cases of a herniated disc, a fragment from the interior pushes into the spinal canal through a tear or rupture in its outer layer. Since there isn’t room for both the spinal nerve and the displaced fragment, it crowds the nerve, resulting in sharp shooting pain, numbness and weakness. Herniated discs can occur in any part of the spine, but are most common in the lower back or neck. Lifting something heavy or twisting awkwardly may cause a herniated disc. But so can degeneration and weakening over time. To some degree, herniated discs may be genetic, since they’re more likely to develop if they run in the family.
Sciatica
About as thick as your pinky finger, the sciatic nerve is the largest nerve in your body, running from the lower back through the backs of your thighs and all the way down to your feet. Because of the length of the nerve down your leg, sciatica feels like a sharp, stabbing or burning sensation that radiates down, usually on just one side of the body. Sciatica is another term for “lumbar radiculopathy,” and lumbar refers to the lower back. Sciatic pain can range from soreness, numbness, tingling to electric shock, throbbing heat, or intense stabbing pain.
Whether it’s accompanied by sudden shooting pain or discomfort that continues for months, sciatica occurs when the discs that cushion your lower spine place pressure or compression upon the sciatic nerve. Basically, there is pinching and irritation of the sciatic nerve. Sciatica can also occur from a ruptured disc that bulges outward in the spine, narrowing the spine, which is also known as spinal stenosis.
Pinched nerve in the neck
In the same way a pinched nerve in the lower back can cause sciatica (i.e. lumbar radiculopathy), a pinched nerve in the neck results in cervical radiculopathy. This occurs when a herniated disc at the top of the spine irritates a nerve in the neck to the point of nerve compression. Ouch, right?
Arthritis, or wear-and-tear from aging, can also cause compression. How do you know if you have a pinched nerve in your neck? Well, when you try to move your head from one side to the other, your body will let you know quickly.
However, some key signs of a pinched nerve in the neck include: a sensation of stiffness in the neck and shoulder blades, a pain that shoots or radiates into the shoulder, arm, or fingers, a tingling “pins-and-needles” feeling in the hand or fingers and a weakness or numbness in the arm.
How do you treat a pinched nerve?
When you’re suffering from a pinched nerve, you want relief — and you want it fast. There are many different ways to alleviate your symptoms; from basic exercises and stretches to yoga moves and more, here is what you should consider when suffering from this condition.
We will cover the most common treatment options, including:
- Stretches
- Physical therapy
- At-home remedies
- Yoga
- Prescription painkillers
- Surgery or injection
Stretches
Sciatic pain relief stretches aim to reduce pressure on the sciatic nerve, often by externally rotating the hip. To relieve sciatic nerve pain, examples of stretches include: variations of Pigeon Pose in yoga, glute and hamstring stretches, back extensions and bringing your knee to the opposite shoulder.
To treat a pinched nerve in the neck, you need some basic moves and rest. Exercises like side bends, neck tilts and shoulder rolls can alleviate the tenderness. Posture matters here, too! Try to keep your ears level with the shoulders and your jaw loose instead of clenched to help reduce the pain.
Physical therapy
If you sit at a desk all week and then throw yourself into a workout on the weekend without warming up, you may increase the risk of pinched nerves and back pain. That’s where physical therapy comes in — it’s a way to integrate regular activity into your life. Building strength in muscles can keep them from caving into the compression that causes a pinched nerve.
What’s more, working with a physical therapist can build strength while stretching the muscles in the area of the pinched nerve, easing compression and relieving pressure. This can help relieve pain, make movement more accessible and help you become more flexible and active. Stronger muscles and better flexibility can also prevent pinched nerves, as well as offer sciatic pain relief by creating more robust support for the nerve. In general, bed rest, stretching and physical therapy can all treat pinched nerves by relieving pain and allowing for recovery time.
At-home remedies
Home remedies like cold packs or heating pads can also help the affected pinched nerve area. Anti-inflammatory drugs, nutraceuticals and creams can help manage the associated painful symptoms as well. Corticosteroids, taken by mouth, may help minimize pain and inflammation. You can also wear splints or bands to help you stop moving the pinched nerve area to help promote recovery.
Yoga
By increasing flexibility in your spine, promoting circulation and cultivating a sense of rest and relaxation, the practice of yoga appears to relieve lower back pain, including sciatic pain. In fact, yoga may relieve pain in ways comparable to physical therapy. Elements of yoga practice that may help with pinched nerves include relaxation exercises, deep breathing and yoga poses with props such as chairs, straps and blocks to help with deep stretching. Examples of yoga poses that can treat pinched nerves are: Child’s Pose, Cobra Pose, Locust Pose and Downward Facing Dog. All of these moves aim to lengthen and strengthen the spine.
Prescription painkillers
Painkillers such as non-steroidal anti-inflammatory drugs (NSAIDs) may help reduce swelling and relieve pain for pinched nerves that aren’t severe. However, more potent painkillers, such as opioids, may do more harm than good in the long term by failing to address the root cause while heightening addiction risk.
Surgery or injection
If the pinched nerve doesn't improve after several weeks to a few months, corticosteroid injections may be necessary to minimize pain and inflammation. Corticosteroids are a class of medications that have very strong anti-inflammatory properties. When injected close to the spinal nerve roots, they can help decrease inflammation around nerves and manage pain. If the injection does not do its job, the next step, though not common, would be surgery to remove pressure from the nerve physically. Surgery for a pinched nerve could involve removing bone spurs, extracting a herniated disc from the spine, or even cutting a ligament to create enough room for the nerve. The vast majority of cases will not require surgery.
To relieve the pain of a pinched nerve, it’s best to follow a plan tailored to your individual needs that addresses the root causes of compression, stress and inflammation. Remedies may involve a combination of gentle stretching and movement, strengthening and restorative wellness practices to relieve tension.
The Clearing Solution
If any of the symptoms of a pinched nerve are applicable in your life, know that you do not have to struggle alone. At Clearing, we’re building a comprehensive centralized platform to help you get the relief you need. Depending on your situation, this could include a personalized exercise program, custom compounded pain cream, CBD cream, nutraceuticals, health coaching and access to leading pain specialists.
This article is for informational purposes only and does not constitute professional medical advice. Always seek the advice of your healthcare professional with any questions or concerns you may have regarding your individual needs and medical conditions.